Eating Disorder and GLP-1 Deficiency: Understanding the Complex Relationship
Glucagon-like peptide-1 (GLP-1) receptor agonists have gained significant attention in recent years for their potential in managing type 2 diabetes and weight loss. However, the relationship between GLP-1 deficiency and eating disorders is a complex and understudied area.
What is GLP-1 and How Does it Affect Eating Behaviors?
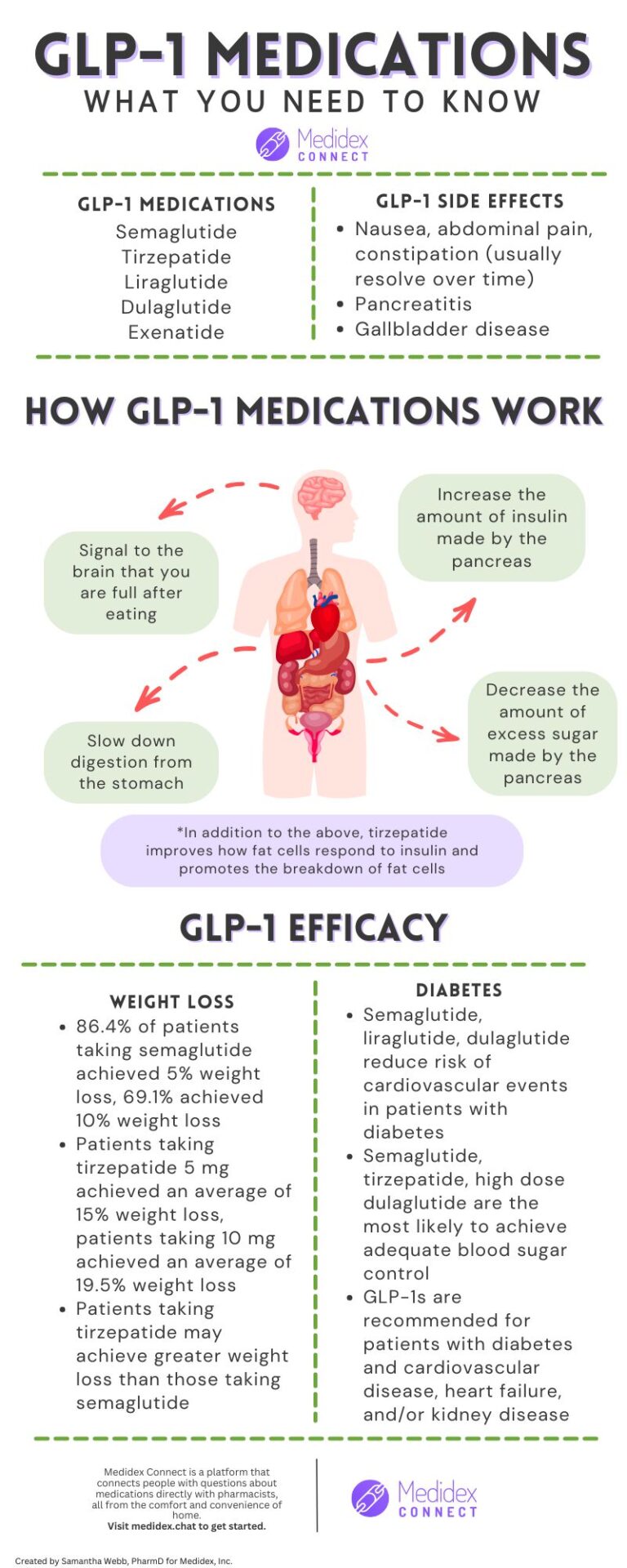
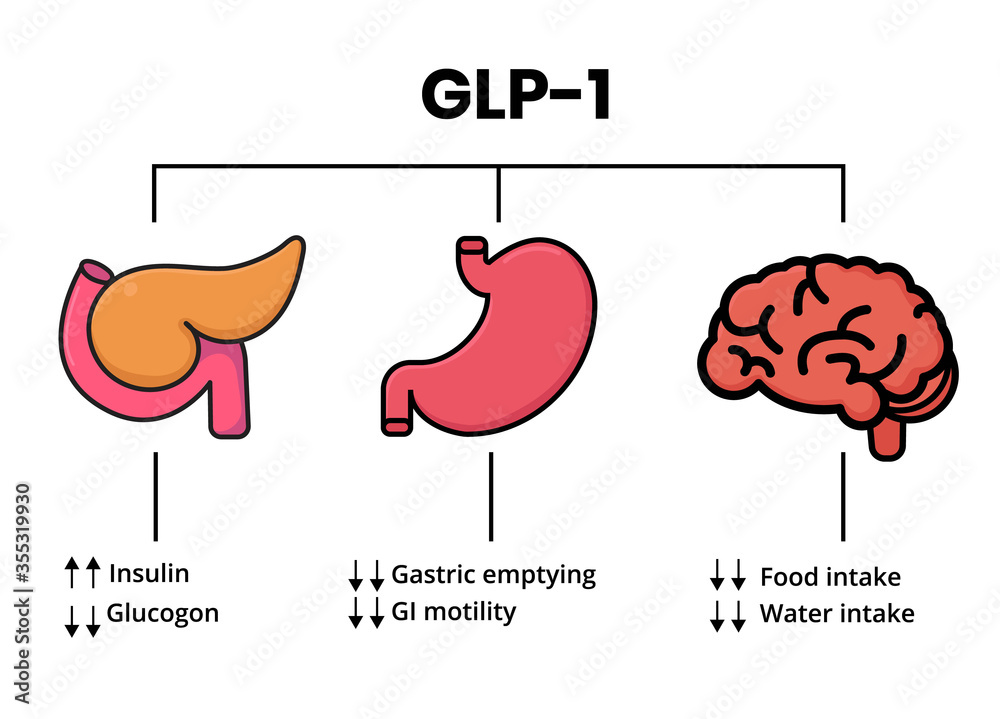
GLP-1 is a hormone produced in the intestines that plays a crucial role in regulating blood sugar levels and appetite. In individuals with eating disorders, the GLP-1 system can be disrupted, leading to abnormal eating behaviors and weight fluctuations.
Research suggests that GLP-1 deficiency may be associated with increased hunger and food intake, particularly in individuals with a history of eating disorders. This is because GLP-1 helps regulate satiety signals in the brain, and a deficiency can lead to an imbalance in these signals, resulting in overeating and weight gain.
Eating Disorder and GLP-1 Deficiency: A Complex Relationship
The relationship between GLP-1 deficiency and eating disorders is complex and bidirectional. On one hand, GLP-1 deficiency may contribute to the development and maintenance of eating disorders. On the other hand, individuals with eating disorders may experience GLP-1 deficiency due to malnutrition, stress, or other factors.
Studies have shown that individuals with anorexia nervosa, bulimia nervosa, and binge eating disorder often have altered GLP-1 levels and function. Additionally, GLP-1 deficiency has been linked to increased risk of developing eating disorders in individuals with a history of trauma or stress.
Risks and Contraindications of GLP-1 Therapy in Eating Disorders

While GLP-1 therapy has shown promise in managing weight and improving glycemic control, it may not be suitable for individuals with eating disorders. The risks and contraindications of GLP-1 therapy in eating disorders include:
- Restrictive eating disorder: Individuals with restrictive eating disorder may experience a worsening of symptoms due to GLP-1 therapy, which can lead to decreased food intake and weight loss.
- Mental health comorbidities: GLP-1 therapy may exacerbate mental health comorbidities, such as depression and anxiety, in individuals with eating disorders.
- Nutrient deficiencies: GLP-1 therapy may increase the risk of nutrient deficiencies, particularly vitamin B12 and iron deficiency, in individuals with eating disorders.
Conclusion
The relationship between GLP-1 deficiency and eating disorders is complex and multifaceted. While GLP-1 therapy has shown promise in managing weight and improving glycemic control, it may not be suitable for individuals with eating disorders. Further research is needed to understand the risks and contraindications of GLP-1 therapy in eating disorders and to develop effective treatment strategies for individuals with co-occurring GLP-1 deficiency and eating disorders.
Recommendations
Individuals with a history of eating disorders who are considering GLP-1 therapy should be referred to an obesity medicine specialist and an eating disorders specialist. Additionally, individuals with eating disorders should be monitored closely for signs of GLP-1 deficiency, such as altered hunger and satiety signals, and should receive regular nutritional counseling to prevent nutrient deficiencies.
Takeaway
The relationship between GLP-1 deficiency and eating disorders is complex and bidirectional. While GLP-1 therapy has shown promise in managing weight and improving glycemic control, it may not be suitable for individuals with eating disorders. Further research is needed to understand the risks and contraindications of GLP-1 therapy in eating disorders and to develop effective treatment strategies for individuals with co-occurring GLP-1 deficiency and eating disorders.