Unlocking the Secrets of GLP-1 and Beta Cell Function Improvement
The human body is a complex machine, with various systems working in sync to maintain overall health and well-being. When it comes to diabetes management, the role of glucagon-like peptide-1 (GLP-1) and beta cell function improvement cannot be overstated. In this article, we will delve into the intricate relationship between GLP-1 and beta cell function, and explore the benefits of using GLP-1-based therapies in type 2 diabetes treatment.
GLP-1 and Beta Cell Function: The Connection
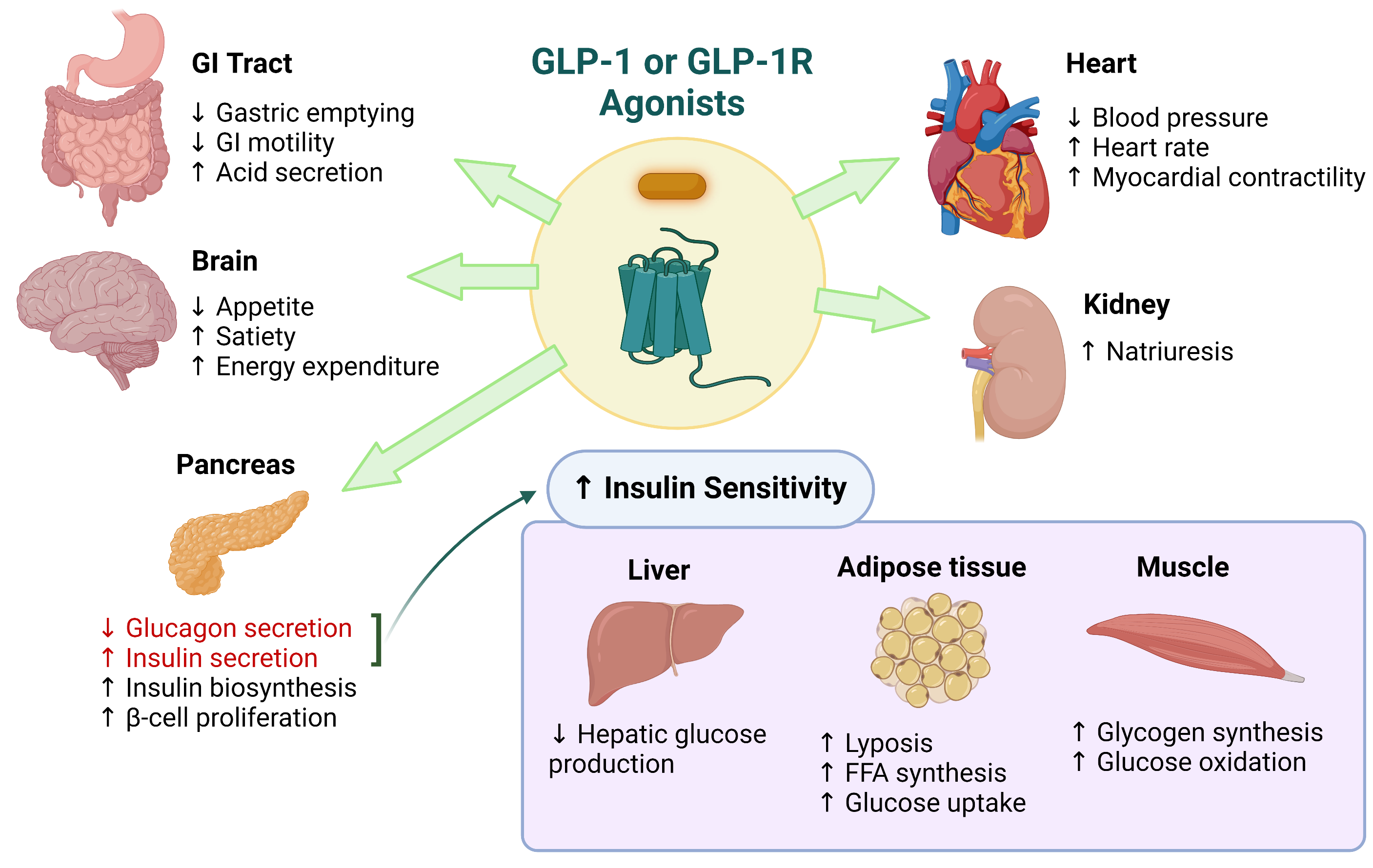
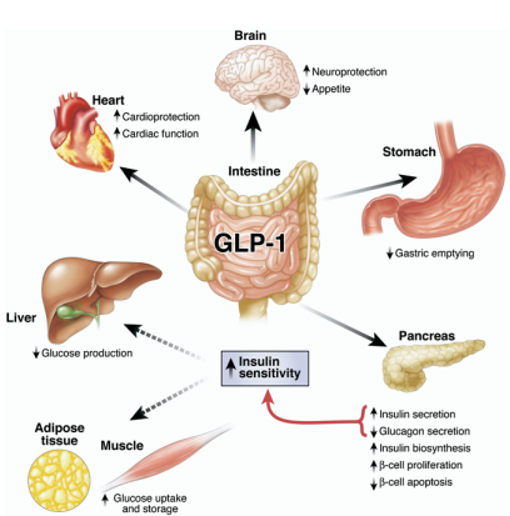
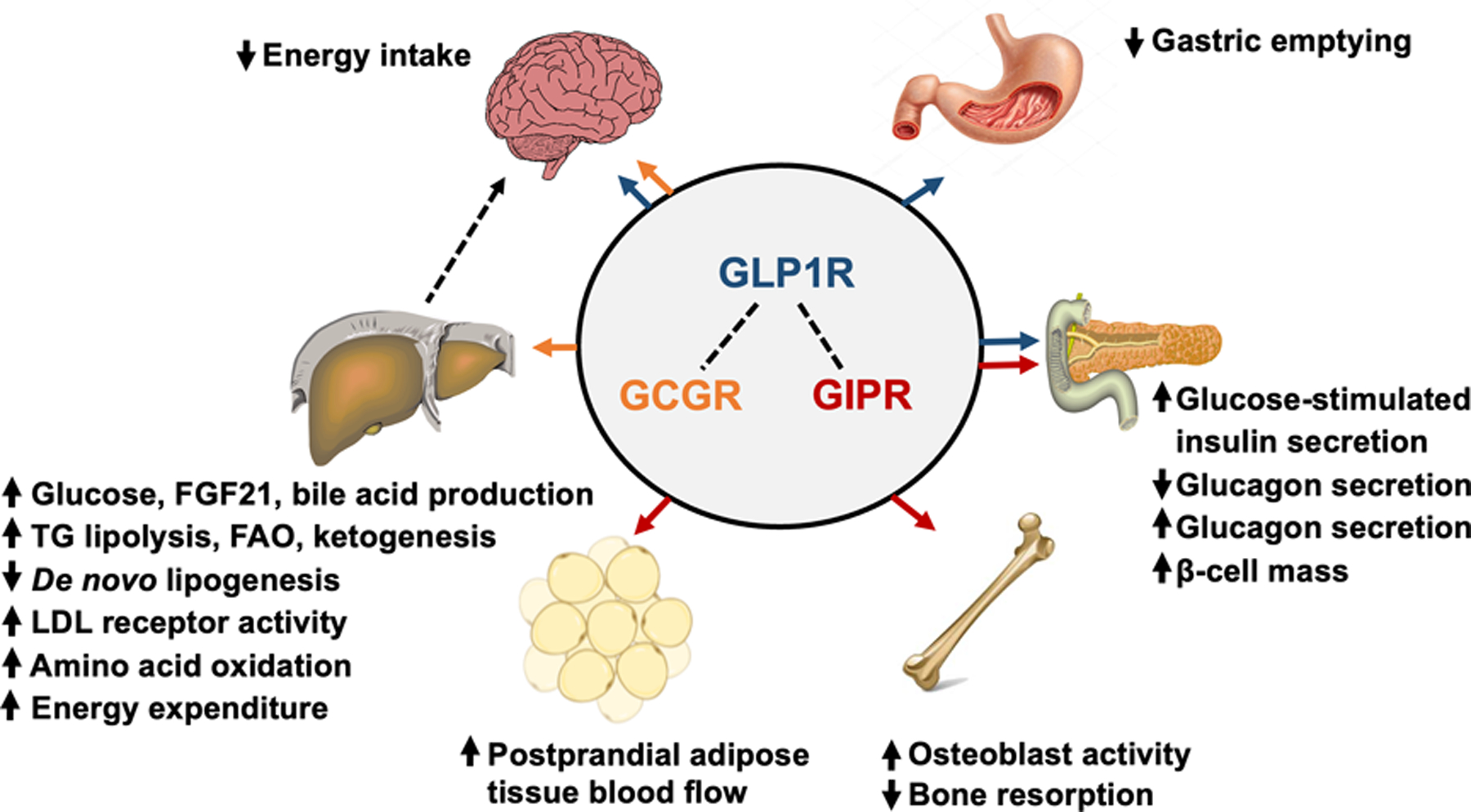
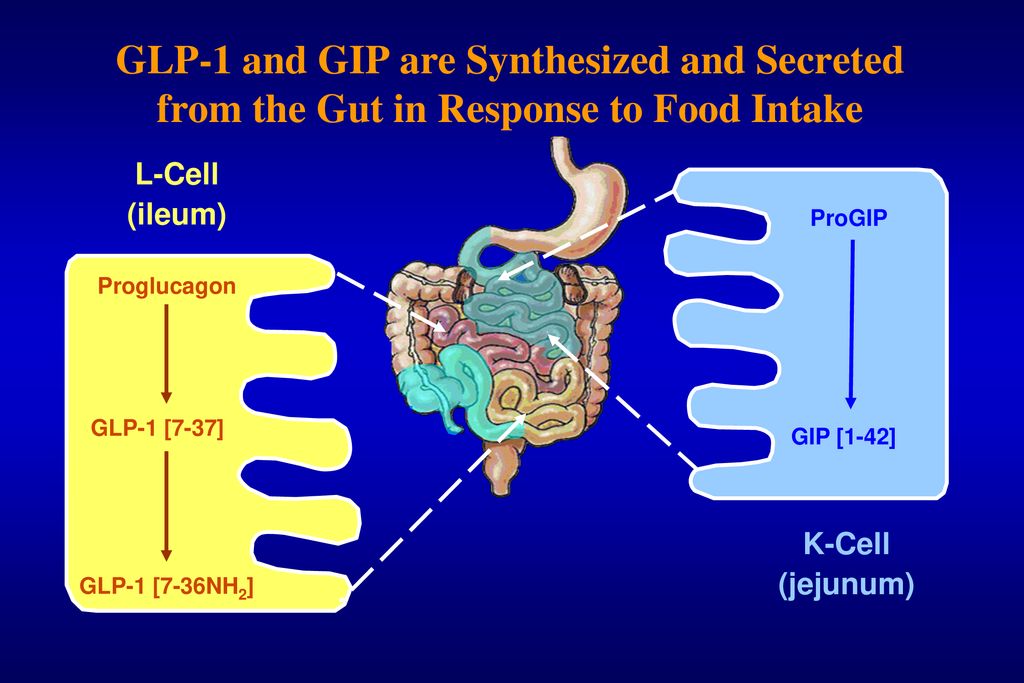
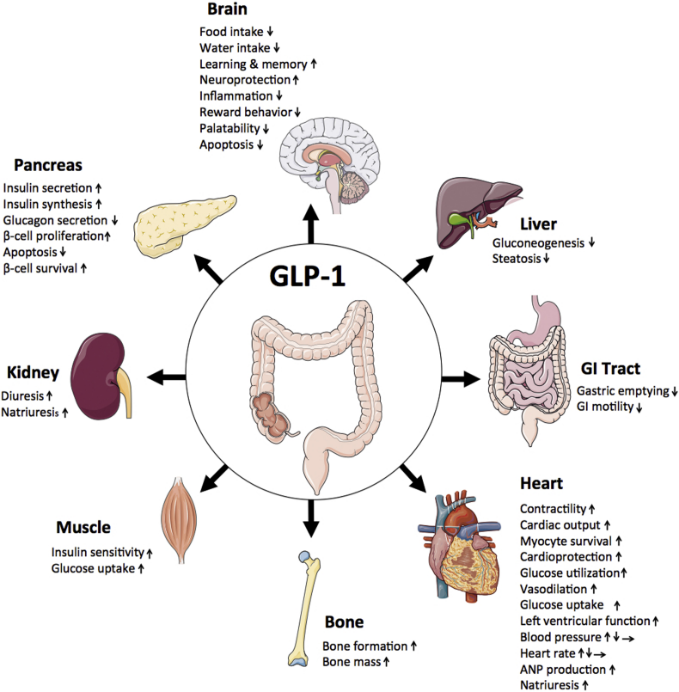
GLP-1 is an incretin hormone secreted by intestinal L cells in response to nutrient intake. It plays a crucial role in glucose homeostasis, enhancing insulin secretion, suppressing glucagon release, reducing appetite, and promoting weight loss. Beyond these effects, GLP-1 also exerts direct effects on the nervous system. The relationship between GLP-1 and beta cell function is multifaceted, with GLP-1 acting as a key player in promoting beta cell growth and protecting them from harm.
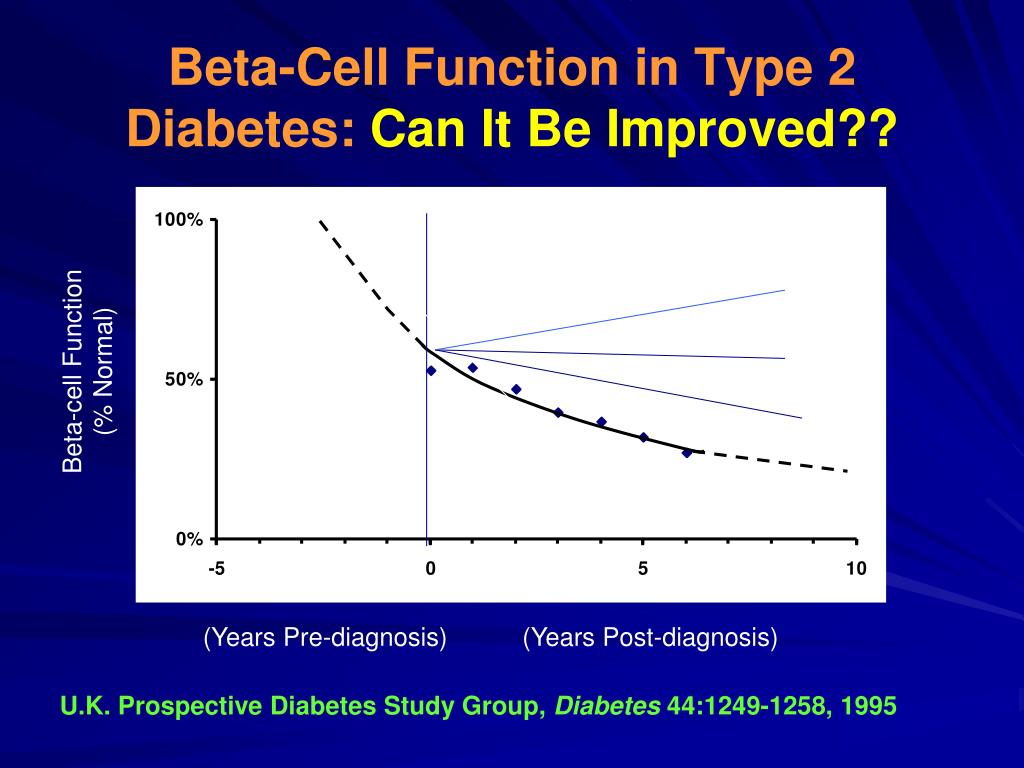
GLP-1 and Beta Cell Function Improvement: The Science Behind It
Studies have shown that GLP-1 receptor agonists (GLP-1RAs) can enhance beta cell function and proliferation, leading to improved insulin secretion and glucose metabolism. GLP-1RAs have been shown to inhibit apoptosis, or programmed cell death, in beta cells, which is a key factor in the development of type 2 diabetes. The therapy has been found to promote beta cell growth and protect against glucotoxicity, a condition in which high glucose levels damage beta cells.
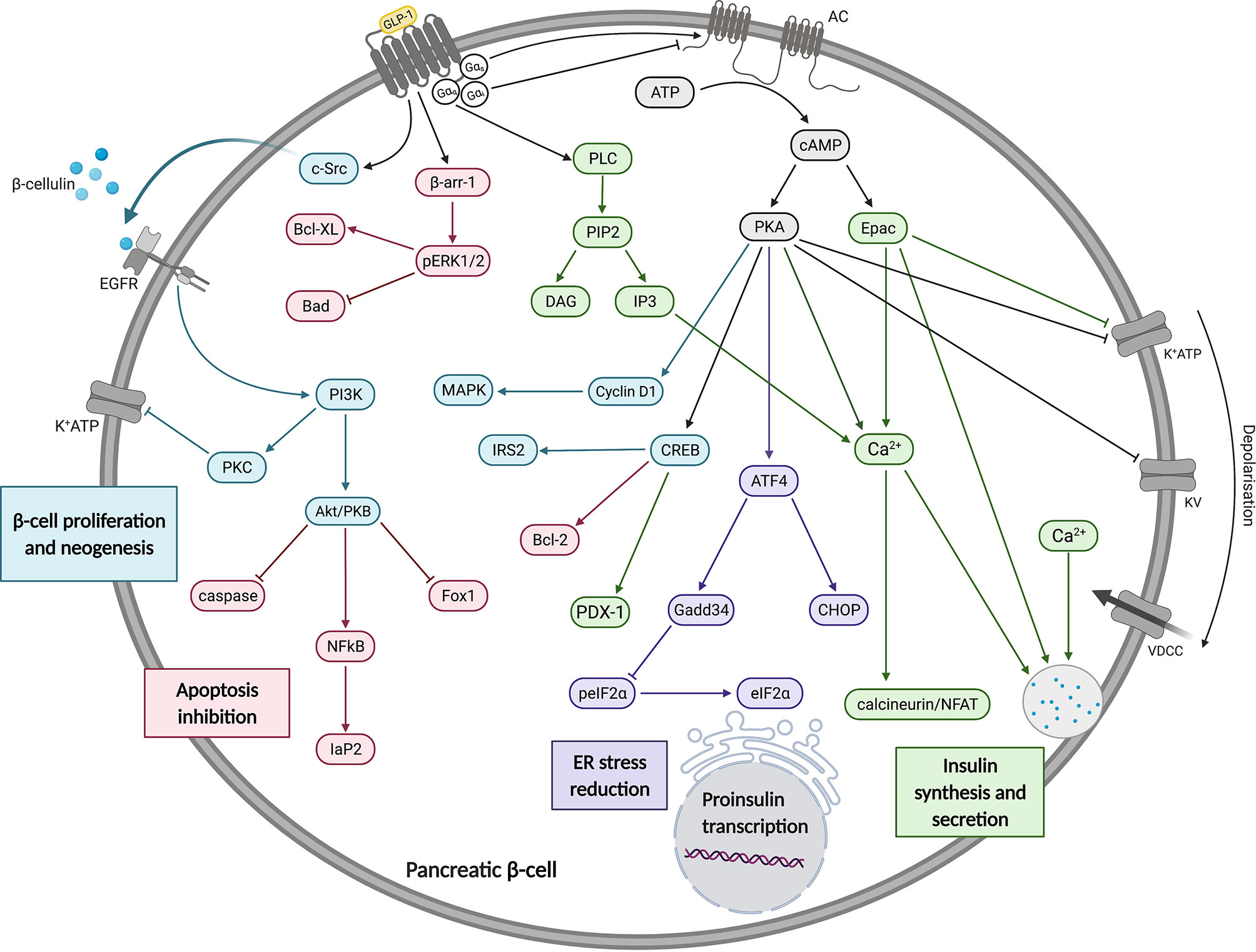
What GLP-1 Does to Beta Cells
- Promotes beta cell growth
- Protects against apoptosis
- Enhances insulin secretion
- Suppresses glucagon release
- Boosts glucose metabolism
GLP-1-Based Therapies in Type 2 Diabetes Treatment
GLP-1-based therapies have emerged as a promising treatment option for type 2 diabetes. These therapies can improve glycemic control, enhance beta cell function, and promote weight loss. They can also reduce the risk of cardiovascular events and nephropathy, making them a valuable adjunct to traditional diabetes management strategies. In cases where beta cell function is preserved, GLP-1 agonists can leverage existing insulin production while offering appetite suppression and weight loss benefits.
How GLP-1 Works in the Body

When you eat, specialized cells release GLP-1, triggering a cascade of effects: your brain receives fullness signals, your stomach empties more slowly, and your pancreas releases insulin more effectively. Semaglutide, for instance, is a modified version of GLP-1 that mimics its effects, slowing gastric emptying and increasing insulin secretion.
Conclusion
GLP-1 and beta cell function improvement hold immense promise in type 2 diabetes management. By understanding the intricate relationship between GLP-1 and beta cell function, healthcare professionals can unlock the secrets of effective diabetes treatment. GLP-1-based therapies can improve glycemic control, enhance beta cell function, and promote weight loss, making them a valuable adjunct to traditional treatment strategies.
References
Nov 26, 2024
Two incretin hormones, glucagon-like peptide-1 (GLP-1) and glucagon-like peptide-2 (GLP-2) glucose stimulated insulin secretory responses in a beta-cell model of diabetes, suggesting potential use as therapeutic agents.
Aug 27, 2025
GLP-1 receptor agonists, such as liraglutide, demonstrate anti-apoptotic effects on pancreatic beta cells in preclinical models, suggesting a potential role in preserving beta cell mass.
Based on these findings, it is clear that GLP-1 plays a vital role in beta cell function and improvement. By exploring its mechanisms and applications in type 2 diabetes treatment, healthcare professionals can provide optimal care and management for their patients.