GLP-1 Benefits for Wound Healing in Diabetes: A Comprehensive Review
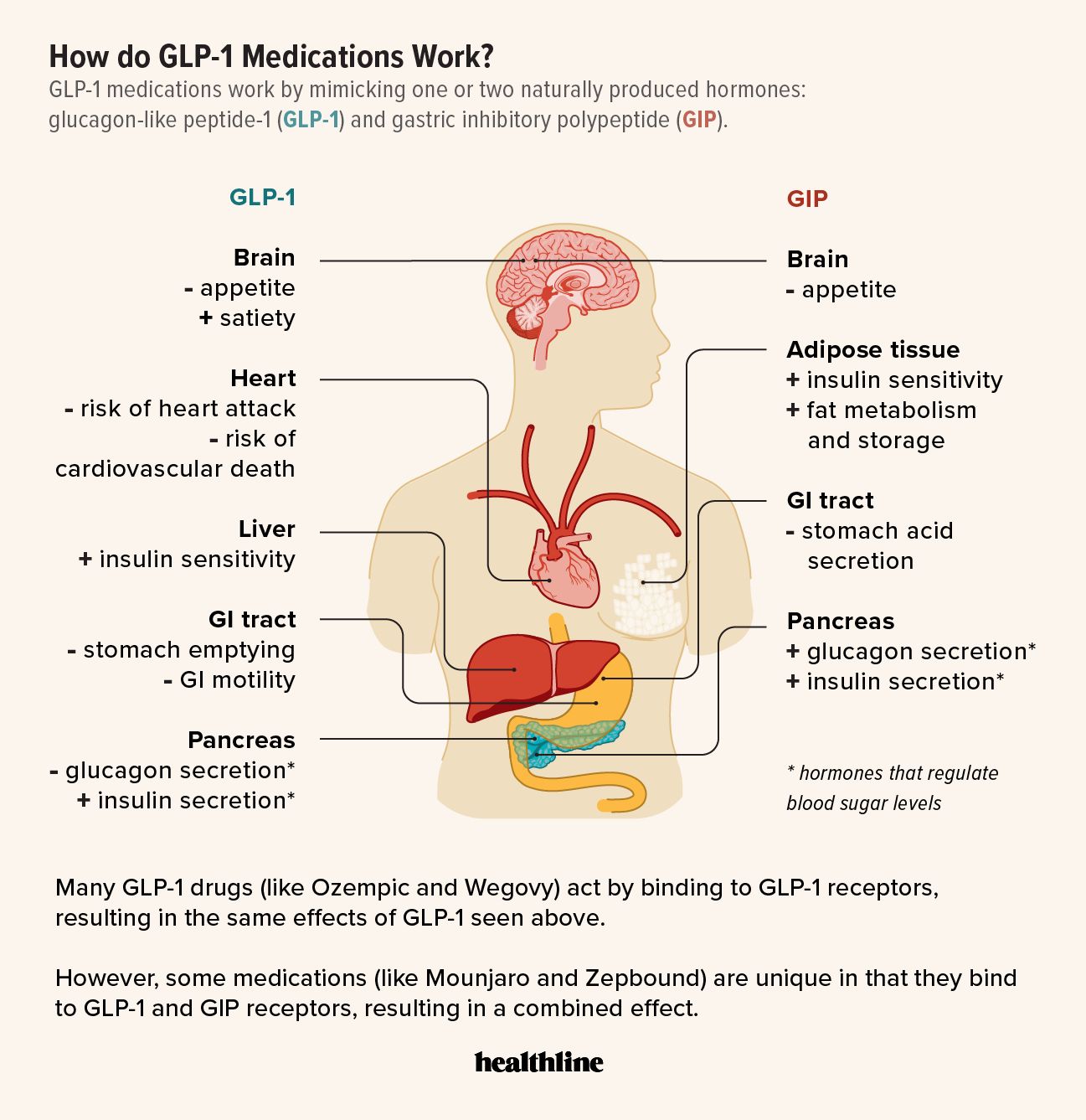
Glucagon-like peptide-1 receptor agonists (GLP-1RAs) have revolutionized the treatment of type 2 diabetes mellitus (T2DM) by improving glycemic control, promoting weight loss, and reducing cardiovascular risk. Beyond their metabolic benefits, GLP-1RAs have been found to have a positive impact on wound healing in diabetic patients. In this article, we will delve into the benefits of GLP-1RAs for wound healing in diabetes and explore the underlying mechanisms.
The High Incidence of Non-Healing Wounds in Diabetes
Diabetic foot ulcers (DFUs) are a major complication of diabetes, affecting up to 25% of patients with T2DM. These wounds are often slow to heal, leading to significant morbidity, mortality, and healthcare costs. The lack of effective treatment regimens for managing DFUs has made GLP-1RAs an attractive therapeutic option for promoting wound healing in diabetic patients.
The Role of GLP-1RAs in Wound Healing
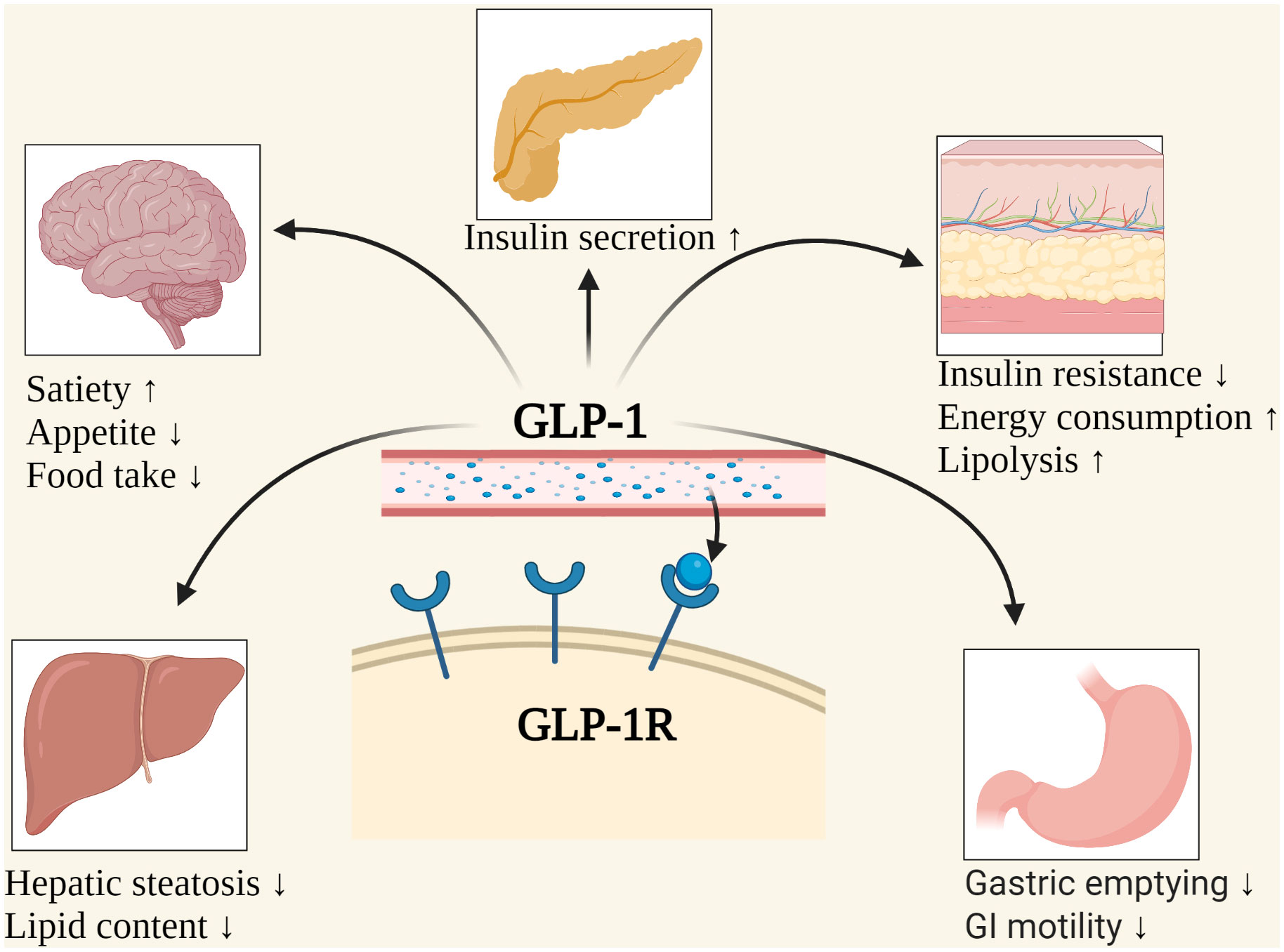
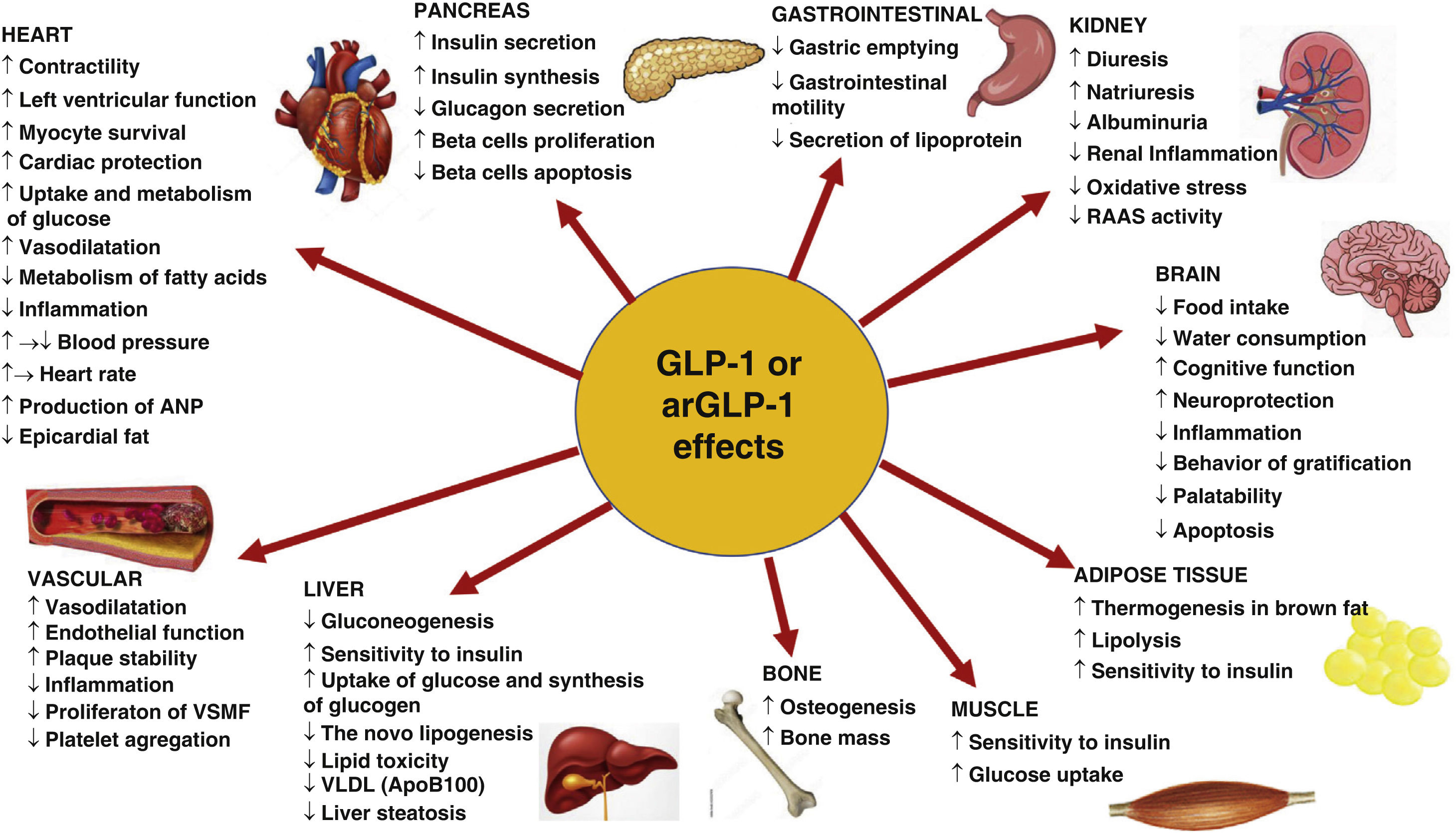
GLP-1RAs have been shown to have beneficial effects on wound healing in several studies. These effects include accelerated wound closure, improved re-epithelialization, and reduced inflammation. The GLP-1 receptor agonists have been found to stimulate the production of growth factors, enhance angiogenesis, and promote tissue repair.
Clinical Studies Supporting the Benefits of GLP-1RAs for Wound Healing
Several clinical studies have demonstrated the efficacy of GLP-1RAs in promoting wound healing in diabetic patients. For example, a study published in the Journal of Foot and Ankle Surgery found that GLP-1 receptor agonists significantly improved wound closure and reduced the risk of amputation in patients with DFUs.
Underlying Mechanisms of GLP-1RAs in Wound Healing
The mechanisms underlying the beneficial effects of GLP-1RAs on wound healing are complex and multifaceted. These effects include the stimulation of growth factors, enhancement of angiogenesis, and reduction of inflammation. Additionally, GLP-1RAs have been found to improve glucose metabolism, which is essential for wound healing.
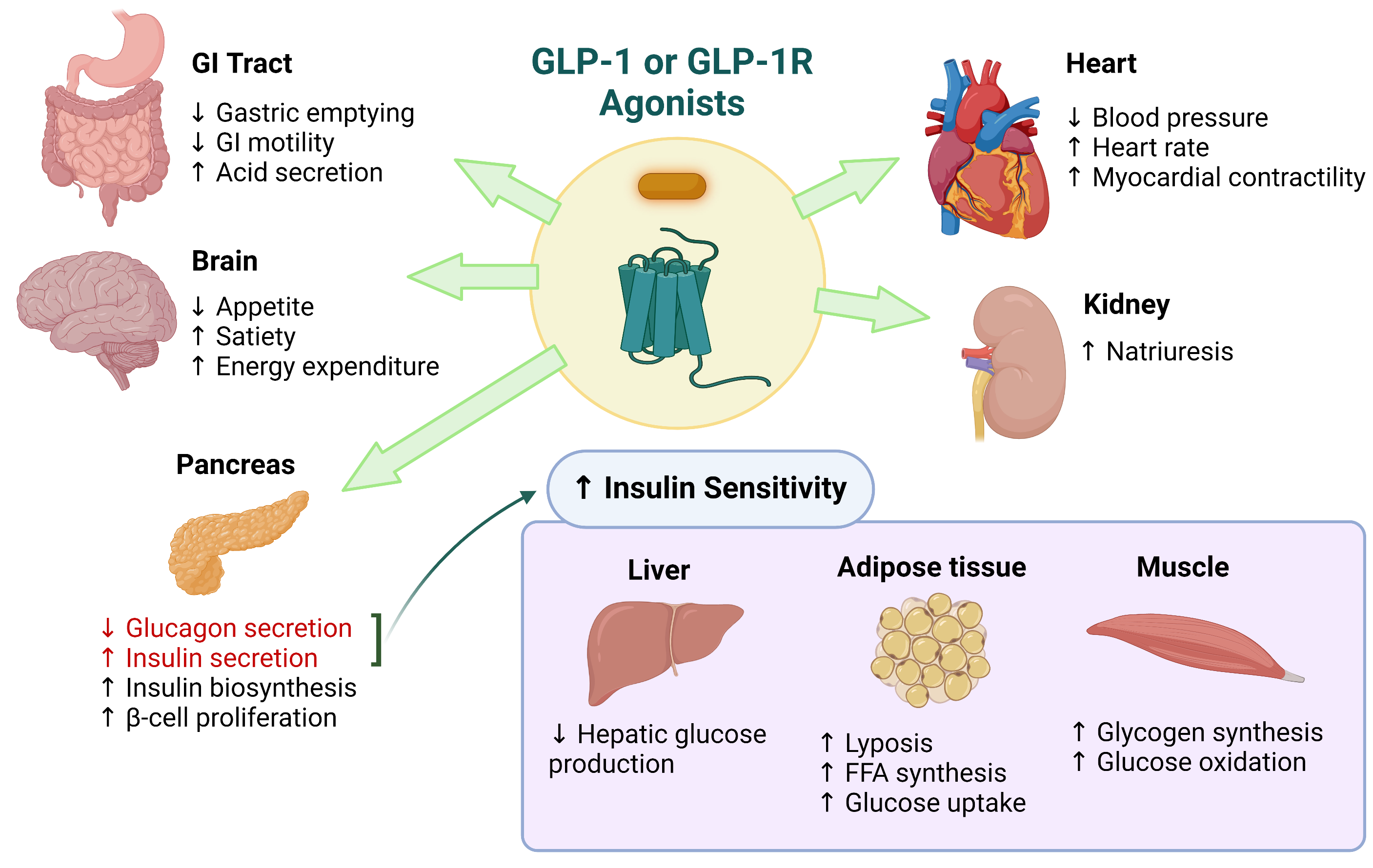
GLP-1RAs and Diabetic Foot Ulcers: A Promising Therapeutic Avenue
GLP-1RAs have emerged as a promising therapeutic option for promoting wound healing in diabetic patients. These agents have been found to have beneficial effects on wound closure, re-epithelialization, and inflammation. Furthermore, GLP-1RAs have been shown to improve glucose metabolism, which is essential for wound healing.
Conclusion
In conclusion, GLP-1RAs have been found to have a positive impact on wound healing in diabetic patients. These agents have been shown to promote wound closure, re-epithelialization, and reduce inflammation. The underlying mechanisms of GLP-1RAs in wound healing are complex and multifaceted, involving the stimulation of growth factors, enhancement of angiogenesis, and reduction of inflammation. Further research is needed to fully elucidate the benefits of GLP-1RAs for wound healing in diabetes.
Future Directions for Research
Despite the promising benefits of GLP-1RAs for wound healing in diabetes, there are several areas that require further research. These include the optimal dosage and duration of treatment, the role of GLP-1RAs in combination with other therapies, and the underlying mechanisms of GLP-1RAs in wound healing. Additionally, further studies are needed to fully elucidate the benefits of GLP-1RAs for wound healing in diabetic patients.
References
- Semaglutide (Ozempic/Wegovy) reduces HbA1c by 1.5-2%, which translates to dramatically better foot wound healing, reduced neuropathy progression, and lower amputation risk in diabetic patients.
- GLP-1 receptor agonists may downregulate inflammatory pathways, enhance wound healing and improve psoriasis severity.
- Dipeptidyl peptidase 4 inhibitors (DPP-4is) have been associated with accelerated wound closure, inhibition of scar formation and a potential reduction in melanoma.
- GLP-1RAs have been found to stimulate the production of growth factors, enhance angiogenesis, and promote tissue repair.